
Join Clinicians Worldwide
Evidence‑based insights to enhance hearing care—twice a month
Subscribe Now
Evidence‑based insights to enhance hearing care—twice a month
Subscribe NowMED-EL
Published Sep 21, 2022
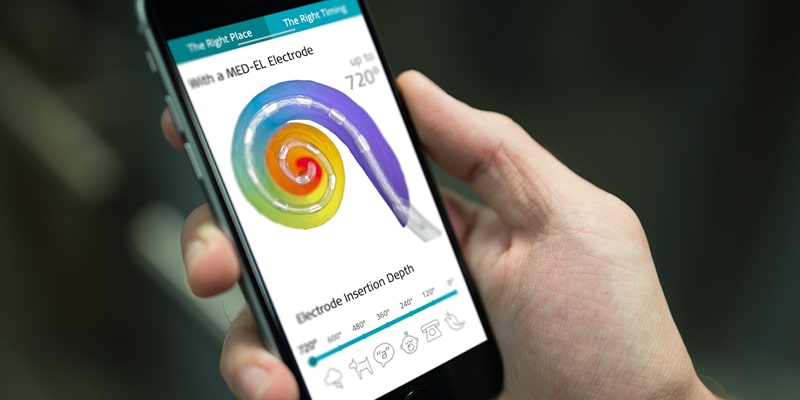
Advances in individualized cochlear implantation, as well as coding and fitting technology, have yielded increasing numbers of recipients who report excellent hearing outcomes, especially in complex listening environments.[18,19,20] But just how close to natural hearing is the sound from a cochlear implant using the latest technology? How is closest to natural hearing achieved, and what benefits can recipients enjoy when it is?
To answer these questions, we would like to share video clips from when we recently interviewed some of the world’s leading experts on these topics.
The first of these experts is Arizona State Prof. Michael Dorman. Dorman and his research team explored how cochlear implant recipients perceive sounds from their MED-EL cochlear implants and how close this is to natural hearing.[1]
The research team asked cochlear implant recipients who have single-sided deafness (i.e., an implanted deaf ear on one side and a normal hearing ear on the other side) to directly compare the sounds of their cochlear implant to sound approximations that were electronically generated. The sound approximations were played to their natural hearing ear until the recipients indicated that the sounds heard in the aided and unaided ears closely resembled each other.
Watch as Prof. Dorman explains the logic behind his research methodology and plays the sound samples that most closely matched what MED-EL recipients hear from their cochlear implants. (Watch until 13:40.)
Can’t see the video? Watch it on YouTube.
The key takeaway here: The longer the electrode array, the more likely a patient will experience a voice quality in the range of normal.
Dorman et al. found that insertion depth, and thus electrode array length, are key factors that influence how likely a patient is to perceive voice quality that sounds normal. According to their findings, when the most apical electrode contact is nearest to tissue around 390 Hz, no shift in formant frequencies is needed to make the sounds match. But when the most apical electrode to stimulate the tissue nearest to electrode contact is around 720 Hz (with about 4 mm less insertion depth), a shift of around +160 Hz is needed to make the sounds match, albeit with lower voice quality.
Through his work with patients with single-sided deafness, Prof. Dorman and his research team also investigated how patients with single-sided deafness perceive the world and how effective cochlear implants are as a treatment for SSD.[2] Watch until 17:24 to find out what he has learned so far.
Can’t see the video? Watch it on YouTube.
Key takeaway here: The world often sounds “distant and tinny” through only one ear. But “the soundstage is broad”, and it sounds like what you remember with one normal hearing ear and one cochlear implant. A large amount of data suggest that music can even sound better when you add an implant to a normal hearing ear.
Recipients can gain more than better sound quality from stimulating the second turn of the cochlea. According to Prof. Paul Van de Heyning, a large amount of research now exists on the impact of stimulating the cochlea’s second turn on the acoustic capabilities of patients.[6,7,8] With the current electrodes available on the market, only the FLEX 28 and FLEXSOFT arrays can stimulate the entire range of the cochlea, and according to Van de Heyning’s research, it yields better speech recognition in noise in daily life and these patients tend to see positive outcomes sooner after the first fitting. Watch until 22:55.
Can’t see the video? Watch it on YouTube.
A key takeaway from Prof. Van de Heyning: “Nature has provided us with a second turn of the cochlea and an apex to perceive low tones.” Thus, stimulating the second turn helps us perceive low tones, rhythms, intonation, knowing if a sentence ends as a statement or a question, or even recognize if a voice is from a male or female speaker.
Van de Heyning noted that since 25% of the spiral ganglion neurons are located in the second turn of the cochlea and extend beyond the basal turn,[3,4,5] clear low frequency perception can only be achieved with a place-dependent stimulation rate and electrodes placed well into the second turn of the cochlea.[3,13,14,15] If the second turn is stimulated, perception of both speech in noise and music quality improve.[12] Watch (until 41:19) as Van de Heyning discusses optimal angular insertion depth in detail:
Can’t see the video? Watch it on YouTube.
Key takeaway: Covering the entire range of the cochlea including the second turn allows a recipient to achieve the closest to natural hearing.
Since human cochleae can vary in size up to 50%, CI electrode arrays are not one-size-fit-all. Matching electrodes to cochlear frequency maps is required for the “optimal fitting and performance of CI recipients.” [3,14,16,17] Watch (until 42:51) as Van de Heyning discusses assessing the size of the cochlea to select the optimal length electrode array for an individual cochlea:
Can’t see the video? Watch it on YouTube.
Key takeaway: Van de Heyning advocates strongly for assessing the size of the cochlea to calculate how long the electrode should be for an individual recipient to reach 650 degrees angular insertion depth. One such tool Van de Heyning recommends for doing so, along with temporal CT scans, is OTOPLAN.
What is the outcome for recipients when cochlear implantation is done to achieve the closest to natural hearing? Roy Smith, who experienced gradual bilateral hearing loss for about 35 years starting around the age of 30, received sequential bilateral cochlear implants. Watch (until 49:53) as Roy describes his experiences being a musician with deafness, hearing aids, and cochlear implants:
Can’t see the video? Watch it on YouTube.
After his implantations, Roy was able to perform in ways not possible when he had his hearing aids. To find out what he gained and what limitations he still experiences, watch (until 51:27) as Roy describes these in detail:
Can’t see the video? Watch it on YouTube.
For more from the experts on the closest to natural hearing and music perception, check out our Music Special Session of ExpertsONLINE: Sound and Music Perception With Cochlear Implants. MED-EL’s signal processing expert Peter Nopp and professors Paul Van De Heyning, Meg Dillon, and Michael Dorman discussed pitch matching, cochlea coverage, coding strategies, and how to achieve closest to natural hearing on October 6, 2022.
Can’t see the video? Watch it on YouTube.
This was part of the upcoming Sound Sensation music festival hosted by MED-EL celebrating the musical talents of hearing implant users. To view the videos, go to: https://hearlife.medel.com/campaigns/sound-sensation/
Don’t miss more articles like this one. Subscribe to the MED-EL Professionals Blog now.
MED-EL
Was this article helpful?
Thanks for your feedback.
Sign up for newsletter below for more.
Thanks for your feedback.
Please leave your message below.
CTA Form Success Message
Send us a message
Field is required
John Doe
Field is required
name@mail.com
Field is required
What do you think?
The content on this website is for general informational purposes only and should not be taken as medical advice. Please contact your doctor or hearing specialist to learn what type of hearing solution is suitable for your specific needs. Not all products, features, or indications shown are approved in all countries.
MED-EL
Get the latest research and resources to help people with every kind of hearing loss. Subscribe to the MED-EL Professionals Blog now.
Registration was successful
We’re the world’s leading hearing implant company, on a mission to help people with hearing loss experience the joy of sound.
Find your local MED-EL team
The content on this website is for general informational purposes only and should not be taken as medical advice. Please contact your doctor or hearing specialist to learn what type of hearing solution is suitable for your specific needs. Not all products, features, or indications shown are approved in all countries.


