MED-EL
Published Jun 07, 2018
Why You Should Treat Every Cochlear Implant Candidate as a Hearing Preservation Case
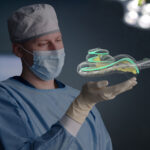
In a recent survey, experienced cochlear implant surgeons reported that they used either lateral wall electrode arrays or perimodiolar electrode arrays in relatively equal numbers in CI cases where “hearing preservation is not a goal”.1
However, nearly 90% of these surgeons prefer a lateral wall electrode array & round window insertion in cases where hearing preservation is a goal. This is logical, as extensive literature has shown that flexible lateral wall arrays enable superior hearing preservation rates as compared to perimodiolar arrays.2,3,4,5,6,16,20,21,22,23
But why is there such a difference in the surgical approach for these two cochlear implant candidates?
Even in profound sensorineural hearing loss, the cochlea is full of living neural structures—a deaf cochlea is not a dead cochlea. If there is trauma during electrode insertion, the natural nerve pathways of the cochlea can be irreversibly damaged.
For the best hearing outcomes, why not treat every cochlear implant candidate as a hearing preservation case? Every cochlear implant recipient should be able to experience the benefits of atraumatic electrode array insertion and structure preservation.
- Preservation of essential neural structures
- Accurate electrode placement7
- Significantly better speech understanding5,7,8
Today, we’re going to look how electrode array design affects structure preservation—and why atraumatic electrode array insertion should be a priority for every cochlear implant candidate.
Hearing Preservation & Structure Preservation
Often, hearing preservation is the goal when using atraumatic structure preservation surgical techniques. Hearing preservation is one distinct benefit of structure preservation, and post-operative residual hearing is a useful indication that structures have been preserved.
This is because if the electrode array deviates into the scala vestibuli, intracochlear fluids can mix, the endocochlear potential is lost, and the hair cells cannot function. If this occurs, all residual hearing would likely be permanently lost.8
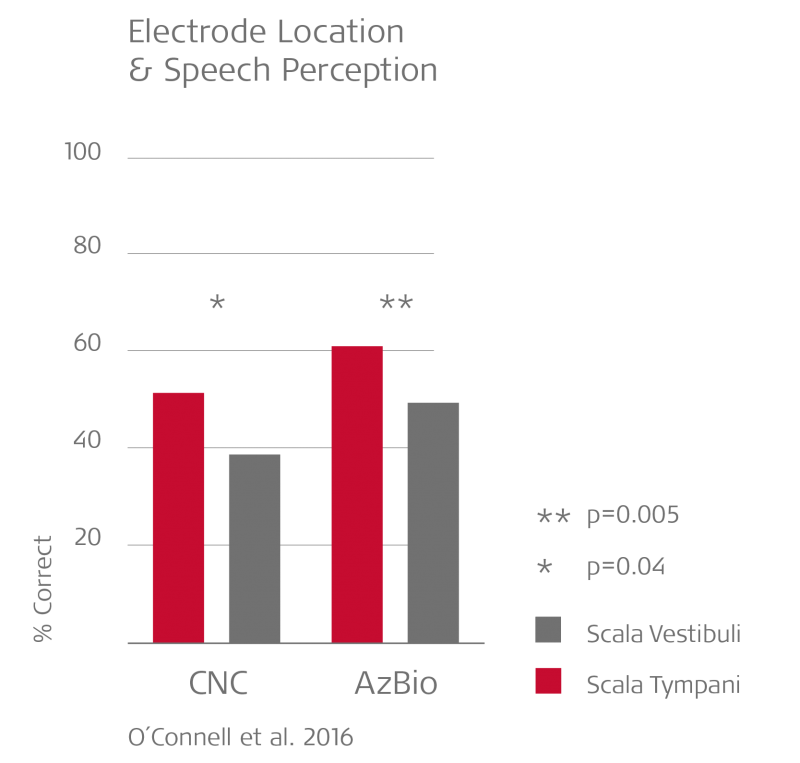
Why should structure preservation and atraumatic insertion be a priority for every candidate? Avoiding trans-scalar deviation enables significantly better hearing performance.2
But even if a candidate has no pre-operative or post-operative residual hearing, they can still benefit from structure preservation techniques. If the electrode deviates into the scala vestibuli, the mix of intracochlear fluids can cause a toxic inflammation that affects the underlying neural structures. By avoiding this damage to neural structures, you can enable significantly better hearing performance.
When the electrode array remains fully in the scala tympani, patients perform significantly better in speech understanding tests. This is why structure preservation should be a priority for every cochlear implant candidate.2,5,7
Perimodiolar vs. Lateral Wall Electrode Arrays
How can you achieve more consistent scala tympani placement? Let’s look at how electrode array choice can affect your patients’ outcomes.
Earlier, we saw how pre-curved perimodiolar arrays can have tip fold-over during insertion, potentially damaging the cochlea and reducing patient benefit. This has been seen in up to 8% of cases with certain pre-curved perimodiolar arrays.9
But there’s an even more prevalent issue with pre-curved perimodiolar arrays—one that can occur in more than 50% of cases. A number of recent studies have shown that perimodiolar & mid-scala electrode arrays are far more likely to deviate through the scala media into the scala vestibuli.2,3,4,5,6
There are several factors that may contribute to this problem with pre-curved perimodiolar arrays: 10
- Stiff electrode array design
- Straight, bundled electrode wires
- A basal stiffening stylet or rigid sheath
- Pre-curved spring design
- Pointed array tip
Trans-scalar deviation with a pre-curved perimodiolar electrode array: The tip of the electrode array punctures from the scala tympani through the scala media into the scala vestibuli, which can cause extensive damage to the osseous spiral lamina, spiral ligament, basilar membrane, and underlying auditory nerve structures.
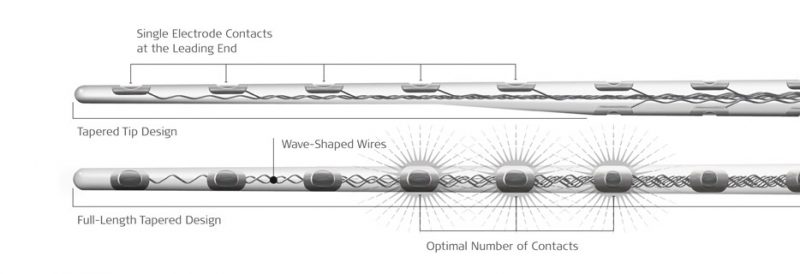 In contrast, scalar deviation can be effectively avoided with MED-EL flexible lateral wall arrays used in combination with structure preservation techniques. With flexible MED-EL lateral wall arrays, the rounded FLEX-Tip design gently deflects away from delicate structures, including the basilar membrane and spiral ligament.
In contrast, scalar deviation can be effectively avoided with MED-EL flexible lateral wall arrays used in combination with structure preservation techniques. With flexible MED-EL lateral wall arrays, the rounded FLEX-Tip design gently deflects away from delicate structures, including the basilar membrane and spiral ligament.
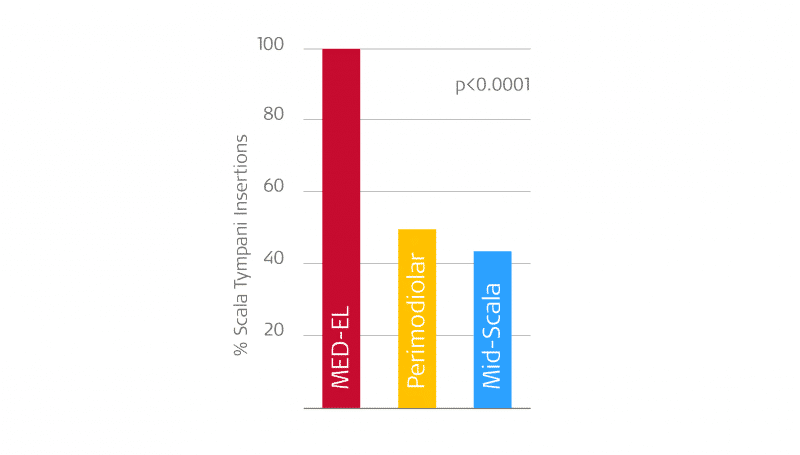
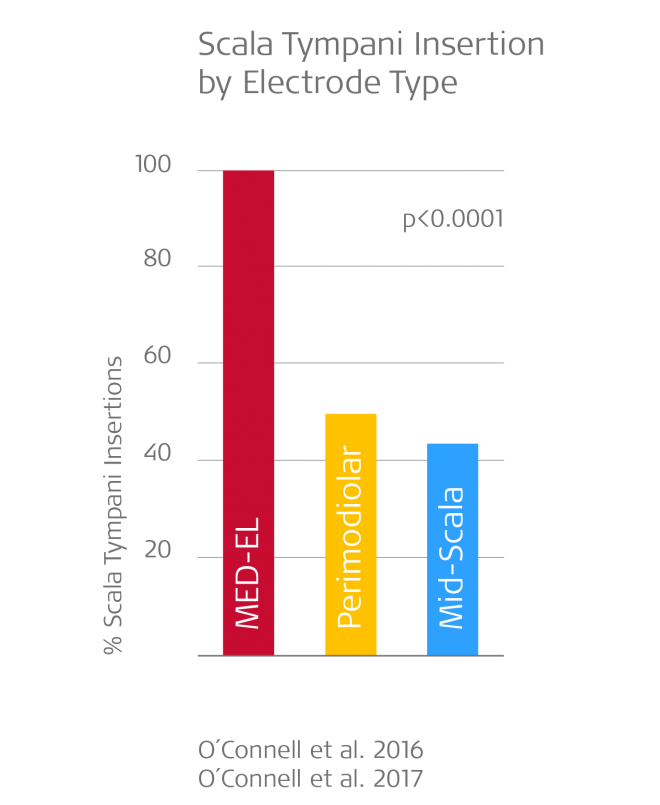 Results from O’Connell et al. (2016 & 2017) that demonstrate that only MED-EL’s flexible lateral wall arrays can provide reliable scala tympani insertion.2,6
Results from O’Connell et al. (2016 & 2017) that demonstrate that only MED-EL’s flexible lateral wall arrays can provide reliable scala tympani insertion.2,6
- Perimodiolar arrays (n=106): only 48.7% fully in scala tympani
- Mid-scala arrays (n=14): only 42.9% fully in scala tympani
- MED-EL lateral wall arrays (n=48): 100% fully in scala tympani
Furthermore, these consistently high structure preservation rates with MED-EL arrays have been independently reported across multiple centers over the past years.
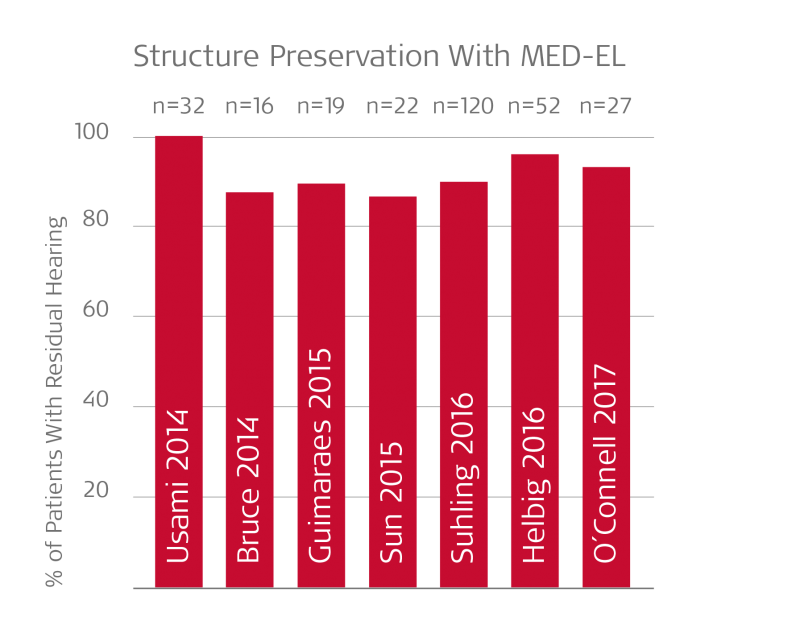 Extensive literature shows consistently reliable structure preservation rates with MED-EL. Graph highlights percentage of patients with measurable post-op residual hearing; rates of successful structure preservation with full scala tympani placement are likely even higher.6,11,12,13,14,15,16
Extensive literature shows consistently reliable structure preservation rates with MED-EL. Graph highlights percentage of patients with measurable post-op residual hearing; rates of successful structure preservation with full scala tympani placement are likely even higher.6,11,12,13,14,15,16
So, in summary, extensive peer-reviewed research has shown:1–17
- Pre-curved perimodiolar electrode arrays are far more likely to damage the cochlea and deviate from the scala tympani into the scala vestibuli. Successful scala tympani placement may be achieved in less than 50% of insertions with these electrode arrays.
- If an electrode array deviates from the scala tympani into the scala vestibuli, the patient will perform significantly worse with their CI. This is true even for patients who had no pre-operative residual hearing.
- MED-EL’s flexible lateral wall arrays can offer consistent scala tympani insertion for optimal hearing performance.
And with MED-EL’s full-length flexible arrays, your patients can also benefit from:2,18,19
- Complete cochlear coverage
- More natural place-pitch match
- Much more natural sound quality
- Significant improvement in hearing in short time
- Significantly better hearing in noise & quiet
Preserving cochlear structures and ensuring scala tympani insertion has proven benefits—and that’s why you should treat every cochlear implant candidate as a hearing preservation case.
Subscribe & Share
Ready to learn more about what makes MED-EL electrode arrays the right choice for your patients?
Take a detailed look at what makes our FLEX arrays the most atraumatic cochlear implant arrays available.
See why only our full-length arrays can provide the closest to natural sound quality.
Find out why natural place-pitch match makes MED-EL the best option for bimodal candidates.
Or, watch this excellent HD surgical case study with Prof. Dr. Paul Van de Heyning and see his structure preservation surgical techniques in incredibly clear HD video.
*Not all products, indications, and features shown are available in all areas. Please contact your local MED-EL representative for more information.
References
- Carlson, M., O’Connell, B., Lohse, C., Driscoll, C., & Sweeney, A. (2018) Survey of the American Neurotology Society on cochlear implantation: Part 2, surgical and device-related practice patterns. Otol Neurotol. 39 (1):e20-e27.
- O’Connell, B.P., Cakir, A., Hunter, J.B., Francis, D.O., Noble, J.H., Labadie, R.F., Zuniga, G., Dawant, B.M., Rivas, A., & Wanna, G.B. (2016). Electrode location and angular insertion depth are predictors of audiologic outcomes in cochlear implantation. Otol Neurotol. 37(8):1016–1023.
- Nordfalk, K., Rasmussen, K., Hopp, E., Bunne, M., Silvola, J.T., & Jablonski, G.E., (2016). Insertion Depth in Cochlear Implantation and Outcome in Residual Hearing and Vestibular Function. Ear Hear. 37(2):e129–137.
- Boyer, E., Karkas, A., Attye, A., Lefournier, V., Escude, B., & Schmerber, S. (2015) Scalar localization by cone-beam computed tomography of cochlear implant carriers: A comparative study between straight and periomodiolar precurved electrode arrays. Otol Neurotol. 36(3):422–429.
- Wanna, G.B., Noble, J.H., Carlson, M.L., Gifford, R.H., Dietrich, M.S., Haynes, D.S., Dawant, B.M., & Labadie, R.F. (2014). Impact of electrode design and surgical approach on scalar location and cochlear implant outcomes. Laryngoscope. 124(6):1–7.
- O’Connell, B., Hunter, J., Haynes, D., Holder, J., Dedmon, M., Noble, J., Dawant, B., Wanna, G. (2017) Insertion depth impacts speech perception and hearing preservation for lateral wall electrodes. Laryngoscope. 127(10):2352–2357
- Holden, L.K, Finley, C.C., Firszt, J.B., Holden, T.A., Brenner, C, Potts, L.G., Gotter, B.D., Vanderhoof, S.S., Mispagel, K., Heydebrand, G., & Skinner, M.W. (2013). Factors affecting open-set word recognition in adults with cochlear implants. Ear Hear. 34(3):342–360.
- O’Connell, B.P., Hunter, J.B., & Wanna, G.B., (2016). The importance of electrode location in cochlear implantation. Laryngoscope Investigative Otolaryngology, 1: 169–174.
- McJunkin, J.,L., Durakovic, N., Herzog, J., & Buchman, C.,A. (2018) Early Outcomes With a Slim, Modiolar Cochlear Implant Electrode Array. Otol Neurotol. 39(1):e28-e33.
- Dhanasingh, A. & Jolly, C. (2017) An overview of cochlear implant electrode array designs. Hear Res.356: 93–103.
- Usami, S., Moteki, H., Tsukada, K., Miyagawa, M., Nishio, S.Y., Takumi, Y., Iwasaki, S., Kumakawa, K., Naito, Y., Takahashi, H., Kanda, Y., & Tono, T. (2014). Hearing preservation and clinical outcome of 32 consecutive electric acoustic stimulation (EAS) surgeries. Acta Otolaryngol. 134(7):717–727
- Bruce, I.A., Felton, M., Lockley, M., Melling, C., Lloyd, S.K., Freeman, S.R., & Green, K.M. (2014). Hearing preservation cochlear implantation in adolescents. Otol Neurotol. 35(9):1552–1559.
- Guimarães, A.C., Carvalho, G.M., Duarte, A.S., Bianchini, W.A., Sarasty, A.B., Gregorio, M.F., Zernotti, M.E., Sartorato, E.L., & Castilho, A.M. (2015). Hearing preservation and cochlear implants according to inner ear approach: multicentric evaluation. Braz J Otorhinolaryngol. 81(2):190-196
- Sun, C.H., Hsu, C.J., Chen, P.R., & Wu, H.P. (2015). Residual hearing preservation after cochlear implantation via round window or cochleostomy approach. Laryngoscope. 125(7):1715–1719.
- Suhling, M.C., Majdani, O., Salcher, R., Leifholz, M., Buechner, A., Lesinski-Schiedat, A., & Lenarz, T. (2016) The impact of electrode array length on hearing preservation in cochlear implantation. Otology & Neurotology. 37(8):1006–1015.
- Helbig, S., Adel, Y., Rader, T., Stöver, T., & Baumann, U. (2016). Long-term hearing preservation outcomes after cochlear implantation for electric-acoustic stimulation. Otol Neurotol. 37(9):353–359.
- Ketterer, M., Aschendorff, A., Arndt, S., Hassepass, F., Wesarg, T., Laszig, R., & Beck, R. (2018)
- Buchman, C.A., Dillon, M.T., King, E.R., Adunka, M.C., Adunka, O.F., & Pillsbury, H.C. (2014). Influence of cochlear implant insertion depth on performance: a prospective randomized trial. Otol Neurotol., 35(10), 1773–1779.
- Helbig, S., Helbig, M., Leinung, M., Stöver, T., Baumann, U., & Rader, T. (2015). Hearing preservation and improved speech perception with a flexible 28-mm electrode. Otol Neurotol. 2015 Jan;36(1):34-42.
- Manjaly, J.G., Nash, R., Ellis, W., Britz, A., Lavy, J.A., Shaida, A., Saeed, S.R., & Khalil, S.S., (2018). Hearing preservation with standard length electrodes in pediatric cochlear implantation. Otol Neurotol. 39(9)
- US Food & Drug Administration. (2016). Premarket approval, MED-EL, MED-EL EAS System. P000025/S084.
- US Food & Drug Administration. (2014). Premarket Approval, Cochlear Americas, Nucleus Hybrid L24 cochlear implant system. P130016.
- Nassiri, A.M., Yawn, R.J., Gifford, R. H., Haynes, D.S., Roberts, J.B., Gilbane, M.S., Murfee, J., & Bennett, M.L. (2019). Intraoperative electrically evoked compound action potential (ECAP) measurements in traditional and hearing preservation cochlear implantation. J Am Acad Audiol. 30(10). 918–926.
MED-EL
Was this article helpful?
Thanks for your feedback.
Sign up for newsletter below for more.
Thanks for your feedback.
Please leave your message below.
CTA Form Success Message
Send us a message
Field is required
John Doe
Field is required
name@mail.com
Field is required
What do you think?
The content on this website is for general informational purposes only and should not be taken as medical advice. Please contact your doctor or hearing specialist to learn what type of hearing solution is suitable for your specific needs. Not all products, features, or indications shown are approved in all countries.
MED-EL