MED-EL
Published Nov 22, 2017 | Last Update Jun 21, 2023
FLEX Series: Most Atraumatic Cochlear Implant Electrode Arrays
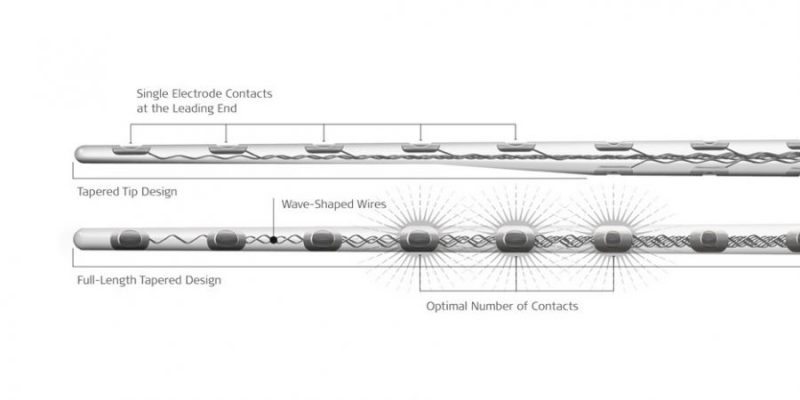
When it comes to choosing a cochlear implant electrode array, atraumaticity should always be a priority. Even for a candidate with no residual hearing, intact cochlear structures are an important factor in hearing performance.
Damage to the cochlea during insertion can significantly affect hearing outcomes. Electrode array deviation into the scala vestibuli can cause loss of natural hearing function, damage to neural structures, pitch confusion, and significantly lower speech perception scores.1,2,3,4,5,6
The cochlea is an incredibly delicate organ, which makes atraumatic electrode arrays an essential consideration for every patient. For more than 30 years, we’ve worked to create the most atraumatic cochlear implant electrode arrays possible.1
Today, we’re going to look at how our FLEX series of electrode arrays offers unparalleled flexibility and atraumaticity that no other electrode array can match.1,4,5,6
FLEX Electrode Arrays
First, let’s look at the general design of our FLEX arrays. Like all MED-EL arrays, the FLEX series are free-fitting lateral wall arrays that can freely adapt to the shape and curvature of each unique cochlea. This free-fitting versatility makes FLEX arrays an excellent option for almost any cochlear implant candidate.
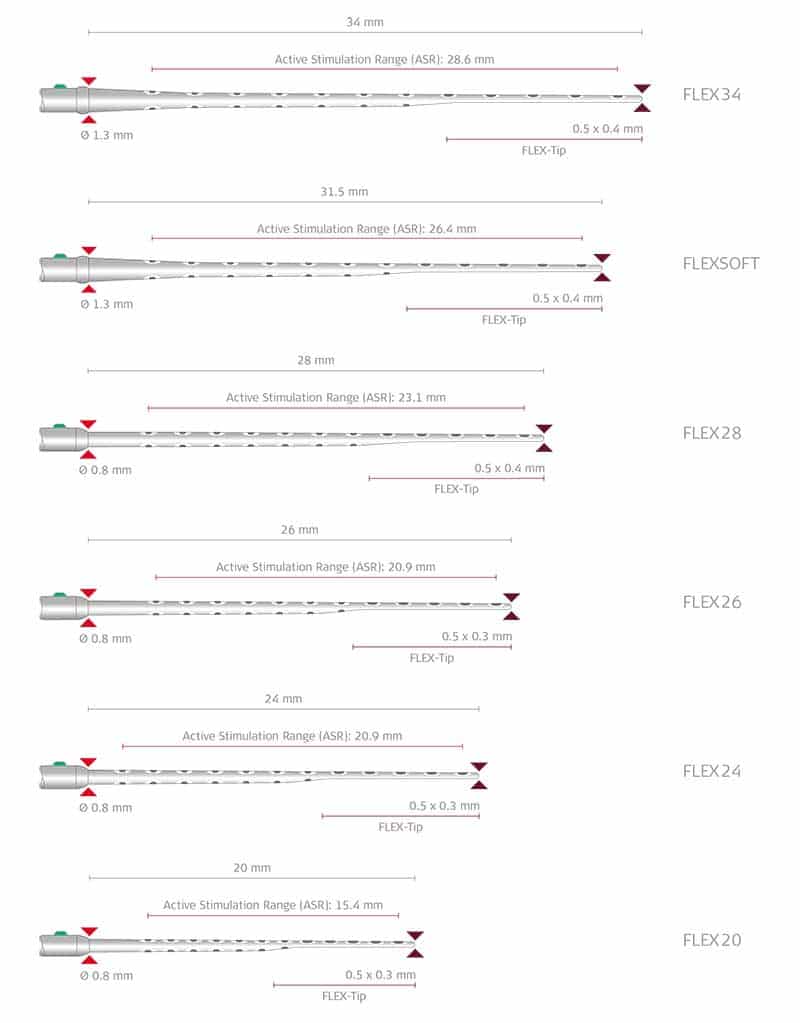
Currently, there are 6 electrodes in the FLEX series:
- FLEX 34: A 34 mm electrode array designed for Complete Cochlear Coverage; the longest FLEX array
- FLEXSOFT: A 31.5 mm electrode array designed for Complete Cochlear Coverage
- FLEX28: A 28 mm electrode array designed for Complete Cochlear Coverage; suitable for 96% of normal cochlear anatomies.7,8
- FLEX26: A 26 mm electrode array designed for Complete Cochlear Coverage
- FLEX 24: A 24 mm electrode array, also designed for Electric Acoustic Stimulation (EAS)
- FLEX 20: A 20 mm electrode array designed for EAS or for other specific needs.
There are 5 key design factors that make FLEX electrode arrays the most atraumatic cochlear implant electrode arrays available.
- Lateral wall array
- Optimized for round window insertion
- Wave-shaped wires
- Optimal contact spacing
- FLEX-Tip technology
No other cochlear implant array available offers this combination. Let’s look at why each factor is so important for overall flexibility and atraumaticity.
Lateral Wall Electrode Arrays
We’ve always used flexible lateral wall arrays because they’re a key factor in atraumaticity. Several recent studies have found that electrode array scalar deviation is far more likely with perimodiolar or mid-scala electrode arrays.1,5,6,9
Pre-curved perimodiolar or mid-scala arrays are designed to curve inward, which can damage delicate structures of the cochlea. These one-size-fits-all perimodiolar electrode arrays are not designed to freely adapt to each unique cochlea.
Round Window Insertion
Surgical approach is also an important factor in hearing preservation. A cochleostomy can lead to a higher likelihood of electrodes in the scala vestibuli. Round window technique has demonstrated much better prospects of having electrodes fully in the scala tympani.5,6,10
Round window insertion has benefits beyond correct scalar placement. In addition to more consistent placement, round window insertion has also been significantly associated with the absence of hydrops and fibrosis of the inner ear in comparison to cochleostomy. A cochleostomy may also cause more acoustic drilling trauma.17,18
Our FLEX electrode arrays are designed for round window insertion. On the FLEX28, FLEX26, FLEX24, and FLEX20, the basal diameter of the electrode is only 0.8 mm, enabling atraumatic insertion without the need for drilling.
Of course, these electrodes can also be inserted using traditional cochleostomy or an extended-round window approach. Surgical flexibility is important, as every patient’s anatomy is unique.
Wave-Shaped Wires
All MED-EL arrays use our unique platinum-iridium wave-shaped wires. Why are wave-shaped wires so important? The waves allow the wires to bend much more easily, which significantly reduces rigidity in comparison to a straight-wire design.

This reduces insertion force and helps minimize the risk of deviating into the scala vestibuli or damaging other cochlear structures.
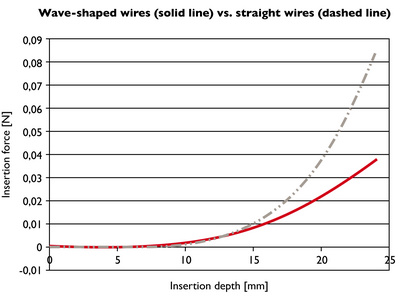
Wave-shaped wires are designed to reduce electrode array insertion force in comparison to straight wires. This approximation shows how wire design may potentially affect insertion forces.
Optimal Contact Spacing
For superior flexibility and sound quality, our electrode arrays use 12 channels spaced evenly along a long electrode array. This minimizes channel interaction and improves mechanical flexibility.
Electrode arrays from other manufacturers use a short electrode array that is densely packed with electrode contacts. This reduces flexibility and also does not offer a natural pitch-place match across the full cochlea.11,14
As we’ve seen before, the most important considerations for sound quality are achieving full cochlear coverage and delivering accurate sound coding. If electrode contacts are spaced too closely together, there’s a chance that two adjacent contacts would stimulate the same set of nerve fibers in the cochlea.
FLEX-Tip Technology
All MED-EL electrode arrays utilize a lateral-wall design, optimal contact spacing, and wave-shaped wires. That’s what makes all MED-EL arrays an excellent choice for atraumatic surgery.
So, what makes FLEX arrays the most atraumatic cochlear implant electrode arrays? That’s where FLEX-Tip technology comes in. Our FLEX arrays have a FLEX-Tip, which uses single contacts at the leading end. Our other electrode arrays use 12 paired electrode contacts along the entire array.
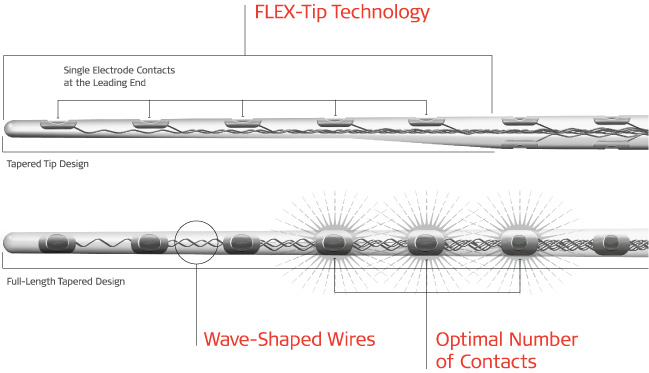
The first 5 apical contacts are single contacts, with the rest of the FLEX array using paired contacts. By using single contacts, the FLEX-Tip of the array is more flexible and can taper down to 0.5 x 0.4 mm (FLEX28). This makes FLEX-Tip exceptionally flexible and atraumatic.
Unlike perimodiolar or mid-scala arrays, the FLEX-Tip is smoothly rounded to avoid catching on intracochlear structures. This flexible tip can gently glide along the scala tympani, avoiding damage to the basilar membrane and other delicate cochlear structures. This makes FLEX electrode arrays an excellent choice for hearing preservation surgery.
Atraumatic Cochlear Implantation
By combining the proven benefits of lateral wall arrays, round window insertion, wave-shaped wires, optimal contact spacing, and FLEX-Tip technology, the FLEX series offers the most flexible and atraumatic cochlear implant electrode arrays available. No other electrode array can match these key design elements.
And the benefits of atraumatic electrode insertion and structure preservation for your patients?
- Accurate electrode mapping 1,2
- Significantly better speech understanding 4,5
- Potential for hearing preservation 10
- Intact cochlear potential for future therapies
And with atraumatic FLEX electrodes, you’re able to insert electrode arrays safely. The benefits of being able to safely insert long electrode arrays?
- “Vocals much more clear and resonant” and “Deeper, more resonant, more natural sound” 11
- Significantly better speech understanding in quiet and noise 12,13
- More natural frequency mapping 14,15
- Significant improvement in speech understanding in a short time 12,16
With a versatile design and exceptional hearing outcomes, FLEX arrays are an ideal choice for nearly every cochlear implant candidate.
Get in Touch
Want to learn more about structure preservation surgical techniques with FLEX arrays? Check out this HD video surgical case study from Prof. Dr. Paul Van de Heyning.
Have a question about structure preservation techniques with cochlear implants? Contact us!
*Not all products, indications, and features shown are available in all areas. Please contact your local MED-EL representative for more information.
References
- O’Connell, B.P., Hunter, J.B., & Wanna, G.B., (2016). The importance of electrode location in cochlear implantation. Laryngoscope Investigative Otolaryngology, 1: 169–174.
- Holden, L.K, Finley, C.C., Firszt, J.B., Holden, T.A., Brenner, C, Potts, L.G., Gotter, B.D., Vanderhoof, S.S., Mispagel, K., Heydebrand, G., & Skinner, M.W. (2013) Factors affecting open-set word recognition in adults with cochlear implants. Ear Hear. 34(3):342–360.
- Nin, F., Hibino, H., Doi, K., Suzuki, T., Hisa, Y., & Kurachi, Y. (2008) The endocochlear potential depends on two K+ diffusion potentials and an electrical barrier in the stria vascularis of the inner ear. Proc Natl Acad Sci USA. 105(5):1751–1756.
- Wanna, G.B., Noble, J.H., Gifford, R.H., Dietrich, M.S., Sweeney, A.D., Zhang, D., Dawant, B.M., Rivas, A., & Labadie, R.F. (2015) Impact of intrascalar electrode location, electrode type, and angular insertion depth on residual hearing in cochlear implant patients: Preliminary results. Otol Neurotol. 36(8):1343–1348.
- Wanna, G.B., Noble, J.H., Carlson, M.L., Gifford, R.H., Dietrich, M.S., Haynes, D.S., Dawant, B.M., & Labadie, R.F. (2014) Impact of electrode design and surgical approach on scalar location and cochlear implant outcomes. Laryngoscope. 124(6):1–7.
- O’Connell, B.P., Cakir, A., Hunter, J.B., Francis, D.O., Noble, J.H., Labadie, R.F., Zuniga, G., Dawant, B.M., Rivas, A., & Wanna, G.B. (2016) Electrode location and angular insertion depth are predictors of audiologic outcomes in cochlear implantation. Otol Neurotol. 37(8):1016–1023.
- Hardy, M. (1938). The length of the organ of Corti in man. J. Anat., 62, 291–311.
- Ni, Y. Dai, P., Dai, C., & Li, H.. (2017) Cochlear implant-related three-dimensional characteristics determined by micro-computed tomography reconstruction. Clin Anat., 30(1), 39–43.
- Boyer, E., Karkas, A., Attye, A., Lefournier, V., Escude, B., & Schmerber, S. (2015) Scalar localization by cone-beam computed tomography of cochlear implant carriers: A comparative study between straight and periomodiolar precurved electrode arrays. Otol Neurotol. 36(3):422–429.
- Nordfalk, K., Rasmussen, K., Hopp, E., Bunne, M., Silvola, J.T., & Jablonski, G.E., (2016). Insertion Depth in Cochlear Implantation and Outcome in Residual Hearing and Vestibular Function. Ear Hear. 37(2):e129–137.
- Harris, R.L., Gibson, W.P. Johnson, M., Brew, J., Bray, M., & Psarros, C. (2011) Intra-individual assessment of speech and music perception in cochlear implant users with contralateral Cochlear and MED-EL systems. Acta Otolaryngol., 131(12), 1270–1278.
- Buchman, C.A., Dillon, M.T., King, E.R., Adunka, M.C., Adunka, O.F., & Pillsbury, H.C. (2014). Influence of cochlear implant insertion depth on performance: a prospective randomized trial. Otol Neurotol., 35(10), 1773–1779.
- O’Connell, B.P., Hunter, J.B., Haynes, D.S., Holder, J.T., Dedmon, M.M., Noble, J.H., Dawant, B.M., & Wanna, G.B. (2017) Insertion depth impacts speech perception and hearing preservation for lateral wall electrodes. Laryngoscope. Epub ahead of print.
- Rader, T., Döge, J., Adel, Y., Weissgerber, T., & Baumann, U. (2016). Place dependent stimulation rates improve pitch perception in cochlear implantees with single-sided deafness. Hear Res., 339, 94–103.
- Vermeire, K., Landsberger, D.M., Van de Heyning, P.H., Voormolen, M., Kleine Punte, A., Schatzer, R., & Zierhofer, C. (2015) Frequency-place map for electrical stimulation in cochlear implants: Change over time. Hear Res., 326,8–14.
- Helbig, S., Helbig, M., Leinung, M., Stöver, T., Baumann, U., & Rader, T. (2015). Hearing preservation and improved speech perception with a flexible 28-mm electrode. Otol Neurotol. 36(1):34-42.
- Ishiyama, A., Doherty, J., Ishiyama, G., Quesnel, A.M., Lopez, I., & Linthicum, F.H. (2016). Post Hybrid Cochlear Implant Hearing Loss and Endolymphatic Hydrops. Otol Neurotol. 37(10):1516–1521.
- Causon, A. Verschuur, C., & Newman, T.A. (2015) A retrospective Analysis of the contribution of reported factors in cochlear implantation on hearing preservation outcomes. Otol Neurotol. 36 (7) 1137–1145
MED-EL
Was this article helpful?
Thanks for your feedback.
Sign up for newsletter below for more.
Thanks for your feedback.
Please leave your message below.
CTA Form Success Message
Send us a message
Field is required
John Doe
Field is required
name@mail.com
Field is required
What do you think?
The content on this website is for general informational purposes only and should not be taken as medical advice. Please contact your doctor or hearing specialist to learn what type of hearing solution is suitable for your specific needs. Not all products, features, or indications shown are approved in all countries.
Roger Bow
January 30, 2024
Are there specific MRI conditions that must be met for scanning Med El flex 24? Thank you, Roger Bow
MED-EL
February 09, 2024
Hi Roger, thank you for your question. Please refer to our Medical Procedure Manual that is included in the implant kit - all our MRI conditions are mentioned there. You can also check our Important Safety Information available in the below link https://www.medel.com/important-safety-information. Kind regards, Gordana
October 01, 2024
I am also looking for this information. I followed the link provided and there is no specific MRI safety information on the Med El flex 28 system. This is to clear the implant for scanning so the Medical procedure manual is not available to us from the implant kit. Please advise where this information can be found.
October 02, 2024
Patricia, thank you for your comment. We would recommend using our Important Safety Information page (https://www.medel.com/important-safety-information) to receive information regarding MRI safety. You can provide your country and system information, and the MRI manual and further resources will show there. Additionally, we would recommend getting in touch with your local MED-EL team as they can take a direct look at your case and provide more information to you. You can get in touch with them here: https://www.medel.com/contact-med-el Kind Regards
Gregor Bertalan
December 09, 2025
I cannot find any MR safety information on the FLEX family in the provided link. Additionally, there is no MR safety information available for the Sonnet3 with FLEX28. This is very frustrating.
MED-EL
December 10, 2025
Hi Gregor, thank you for your comment. You can find important safety information about MED-EL's implant systems here: https://www.medel.com/Important-Safety-Information. Additionally, we would always recommend sharing the link with your medical professional, and letting them know about your cochlear implant and audio processor. Kind Regards
MED-EL

.png)


Conversation
2 Comments