Join Clinicians Worldwide
Evidence-based insights to enhance hearing care—twice a month
Subscribe Now
Evidence-based insights to enhance hearing care—twice a month
Subscribe NowMED-EL
Published Sep 13, 2017

High-frequency hearing loss can be particularly challenging to treat. These patients have minimal hearing loss in the low frequencies (125–1000 Hz), so they are not traditional cochlear implant candidates. However, with severe-to-profound high-frequency hearing loss, hearing aids often do not provide enough benefit. Even with the use of frequency compression or frequency transposition technology in hearing aids, speech understanding can still be very difficult.1,2
That’s why MED-EL created Electric Acoustic Stimulation (EAS) systems to address the specific challenges of high-frequency hearing loss. An EAS system is a two-part approach that combines:
For patients with minimal low-frequency hearing loss and severe-to-profound high-frequency hearing loss, EAS can restore a wide frequency range for optimal hearing outcomes.2,3,4,5,6,7
This week, we’re looking at how EAS can benefit your patients—then we’ll introduce a new expanded indication for MED-EL EAS systems.
First, let’s start by going through a quick overview of how an EAS system works. Our latest EAS system uses the SYNCHRONY cochlear implant and the SONNET EAS audio processor.
Can’t See This Video?
Having problems viewing this video? Watch it on YouTube.
For the cochlear implant, an ultra-flexible electrode array should be gently inserted using hearing preservation surgery techniques to better protect delicate cochlear structures and preserve residual hearing. We generally recommend using the FLEX 24 or FLEX 20 electrode array.2
For acoustic amplification, the SONNET EAS audio processor sends the amplified acoustic signal through the earmold into the ear canal. As our third generation EAS processor, SONNET EAS offers:
The timing of both the electric and acoustic signals are matched, which enables a full, rich perception of sound.
Why should you consider EAS over a high-end hearing aid for your patients? Compared to hearing aids alone, EAS offers significant benefits for recipients with high-frequency hearing loss.2,3,4,5,6,7,8
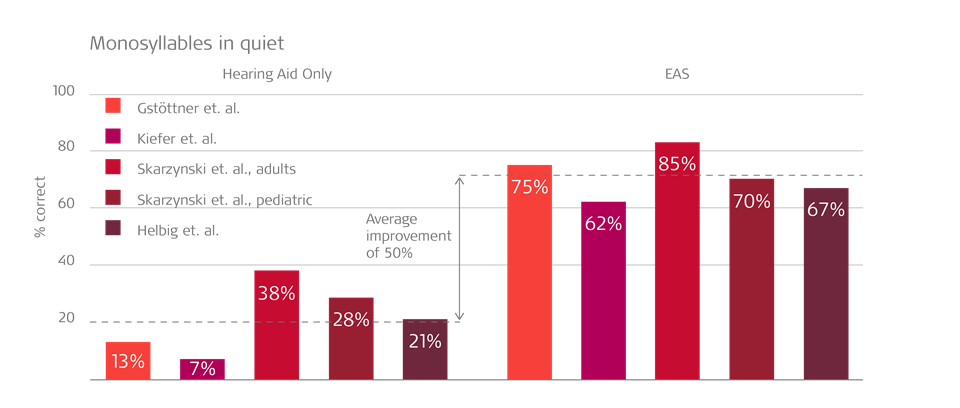 An overview of hearing aid vs EAS hearing outcomes across several studies shows consist benefits.3,4,5,6,7
An overview of hearing aid vs EAS hearing outcomes across several studies shows consist benefits.3,4,5,6,7
How can you determine if a patient is a candidate for EAS? Exact EAS candidacy parameters can vary by country, but these are intended to be used for general guidance.
Indication of sensorineural high-frequency hearing loss with hearing thresholds that fall within the shaded area in the charts below.
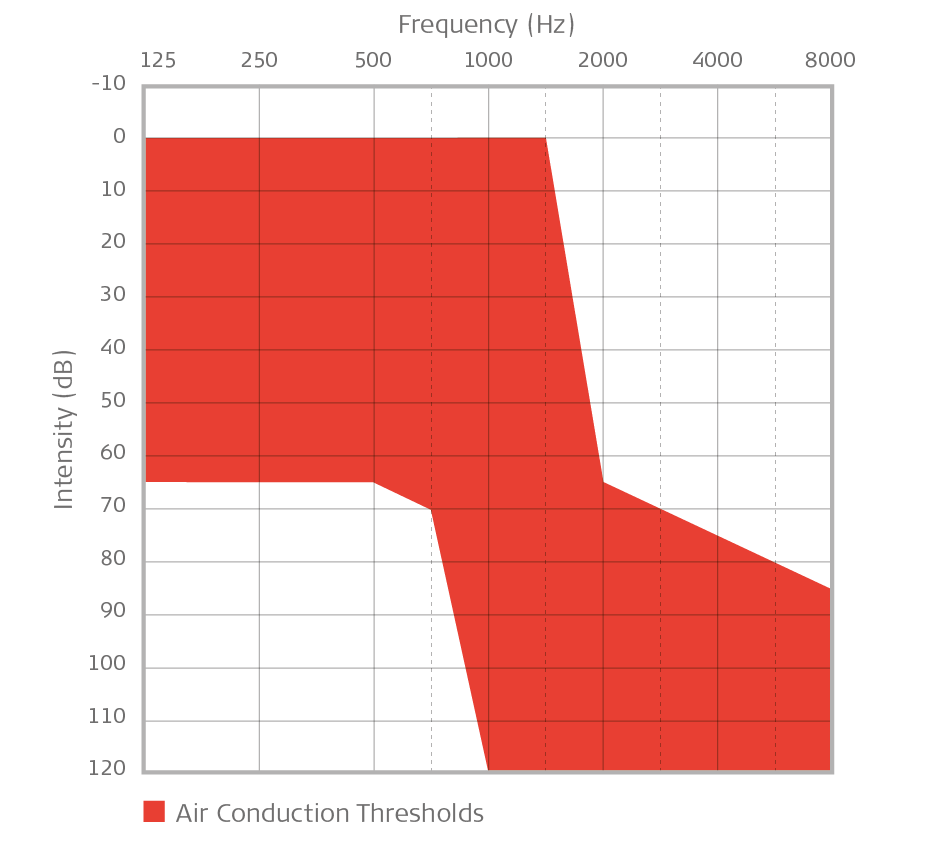 General indication for EAS: Minimal-to-moderate hearing loss up to 750 Hz, sloping down to severe-to-profound sensorineural hearing loss in the higher frequencies. Audiogram should chart within shaded area.
General indication for EAS: Minimal-to-moderate hearing loss up to 750 Hz, sloping down to severe-to-profound sensorineural hearing loss in the higher frequencies. Audiogram should chart within shaded area.
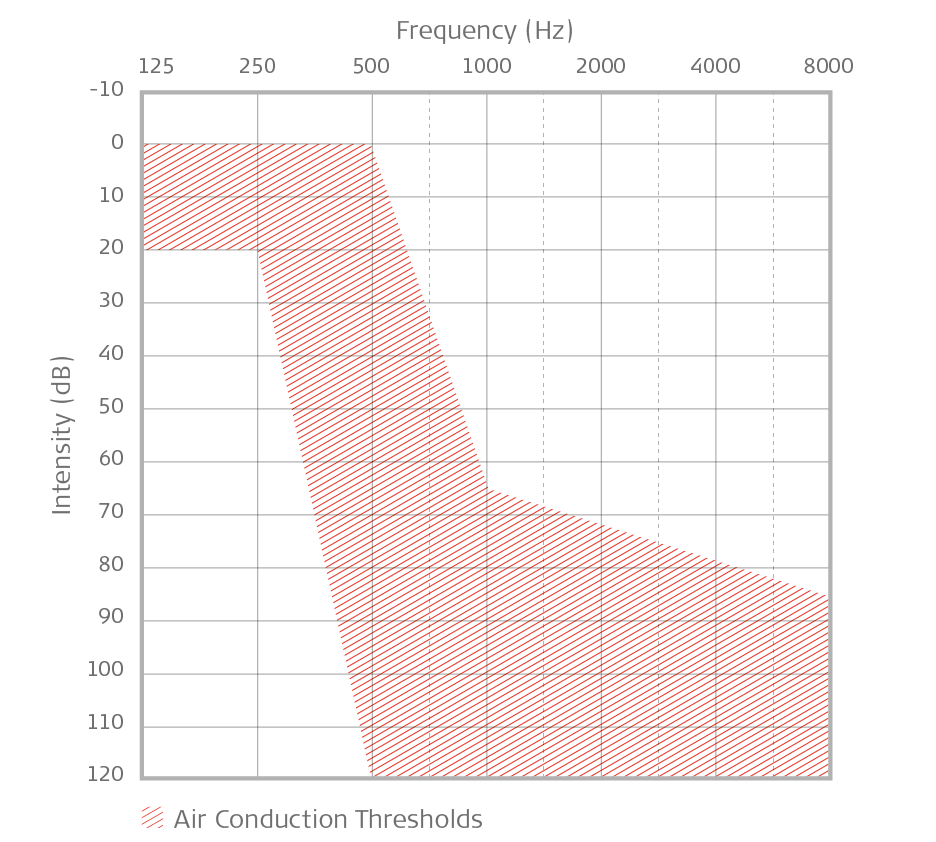
Expanded indication for EAS: No hearing loss up to 250 Hz; at 500 Hz & higher, profound hearing loss. Audiogram should chart within shaded area.
This expanded indication for EAS allows recipients to benefit from their natural residual hearing, even if they have profound hearing loss at 500 Hz and higher on audiometric frequencies.
Of course, natural hearing function is essential for EAS. Yet, every cochlear implantation procedure carries a risk to the delicate cochlear structures and residual hearing.
That’s why MED-EL electrode arrays are designed for superior atraumaticity to protect residual hearing. By combining ultra-flexible lateral wall electrode arrays with round window insertion and hearing preservation techniques, consistently high rates of hearing preservation can be achieved with MED-EL.2,8,9,10,11,12,13,14
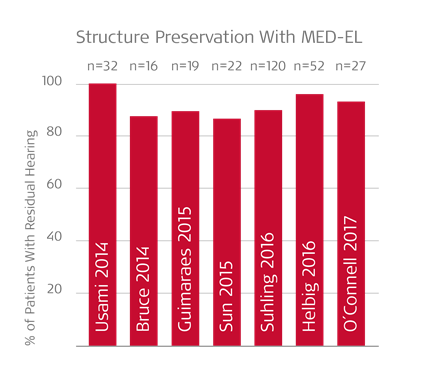
Unfortunately, other “hybrid” systems can often damage or destroy any residual hearing. In the multicenter trial of the Cochlear Nucleus Hybrid L24, 44% of patients completely lost their residual hearing—and a full 10% of patients had to later be reimplanted with a conventional cochlear implant.15
In contrast, in a recent multicenter study of MED-EL EAS systems, 97% of MED-EL recipients were able to use the acoustic component and benefit from EAS.16
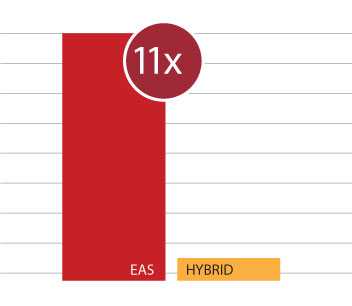
In these studies, MED-EL EAS recipients were 11 times more likely to use their acoustic component after surgery.15,16
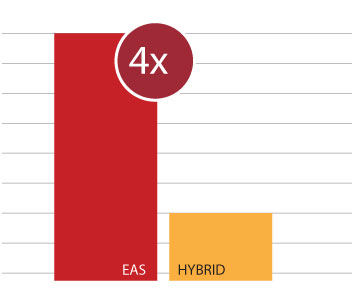
With MED-EL, EAS recipients were 4 times more likely to maintain their residual hearing after surgery.15,16
As you can see, EAS can restore the ability to hear across a wide frequency range, making it an ideal solution for high-frequency hearing loss. The benefits for your patients are significant, including:
And as we’ve shown, MED-EL offers superior outcomes for patients who want to make the most of their natural residual hearing.2,8,15,16
Have a question about EAS for your patients? Leave a comment below or contact us. We’ll have more articles on EAS and hearing preservation—make sure to subscribe now!
References
*Not all products, indications, and features shown are available in all areas. Please contact your local MED-EL representative for more information.
MED-EL
Was this article helpful?
Thanks for your feedback.
Sign up for newsletter below for more.
Thanks for your feedback.
Please leave your message below.
CTA Form Success Message
Send us a message
Field is required
John Doe
Field is required
name@mail.com
Field is required
What do you think?
The content on this website is for general informational purposes only and should not be taken as medical advice. Please contact your doctor or hearing specialist to learn what type of hearing solution is suitable for your specific needs. Not all products, features, or indications shown are approved in all countries.
MED-EL
Get the latest research and resources to help people with every kind of hearing loss. Subscribe to the MED-EL Professionals Blog now.
Registration was successful
We’re the world’s leading hearing implant company, on a mission to help people with hearing loss experience the joy of sound.
Find your local MED-EL team
The content on this website is for general informational purposes only and should not be taken as medical advice. Please contact your doctor or hearing specialist to learn what type of hearing solution is suitable for your specific needs. Not all products, features, or indications shown are approved in all countries.